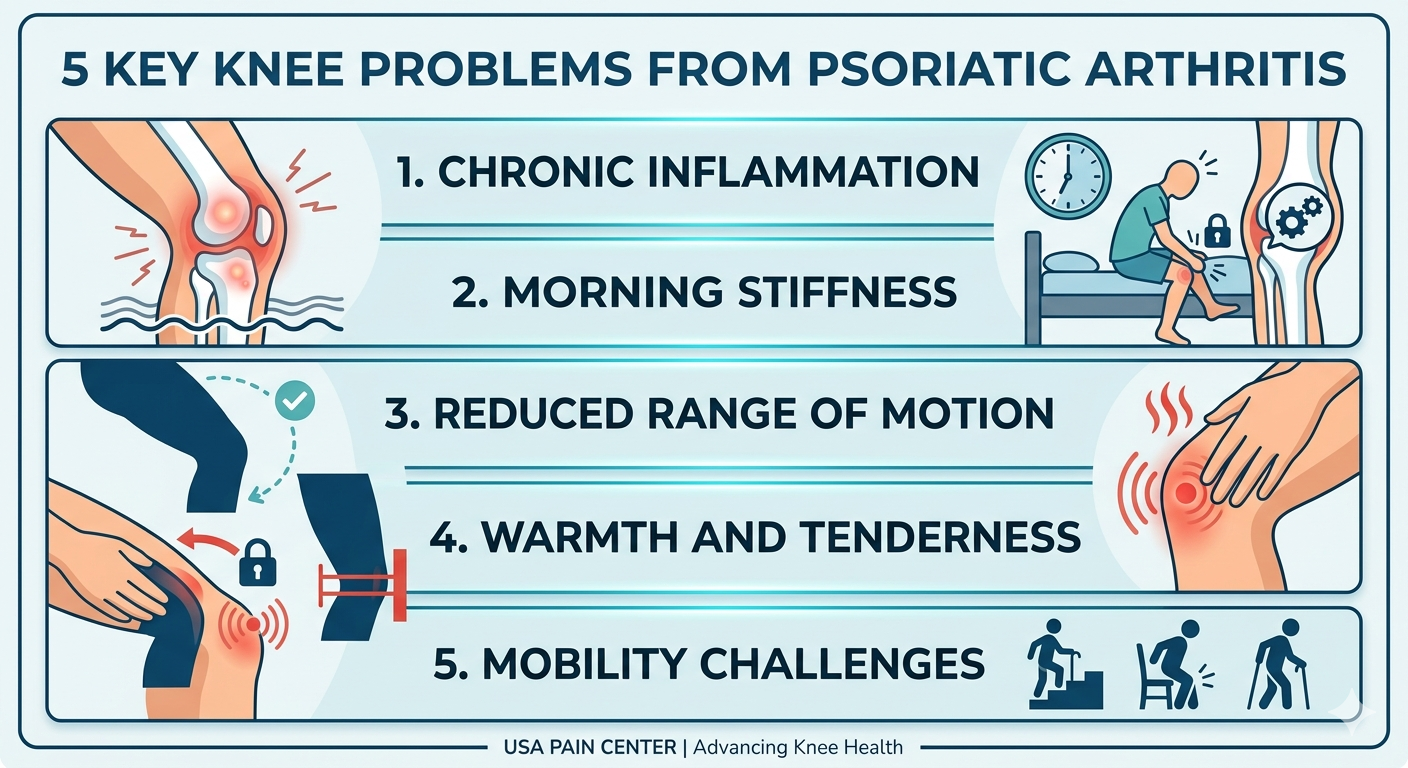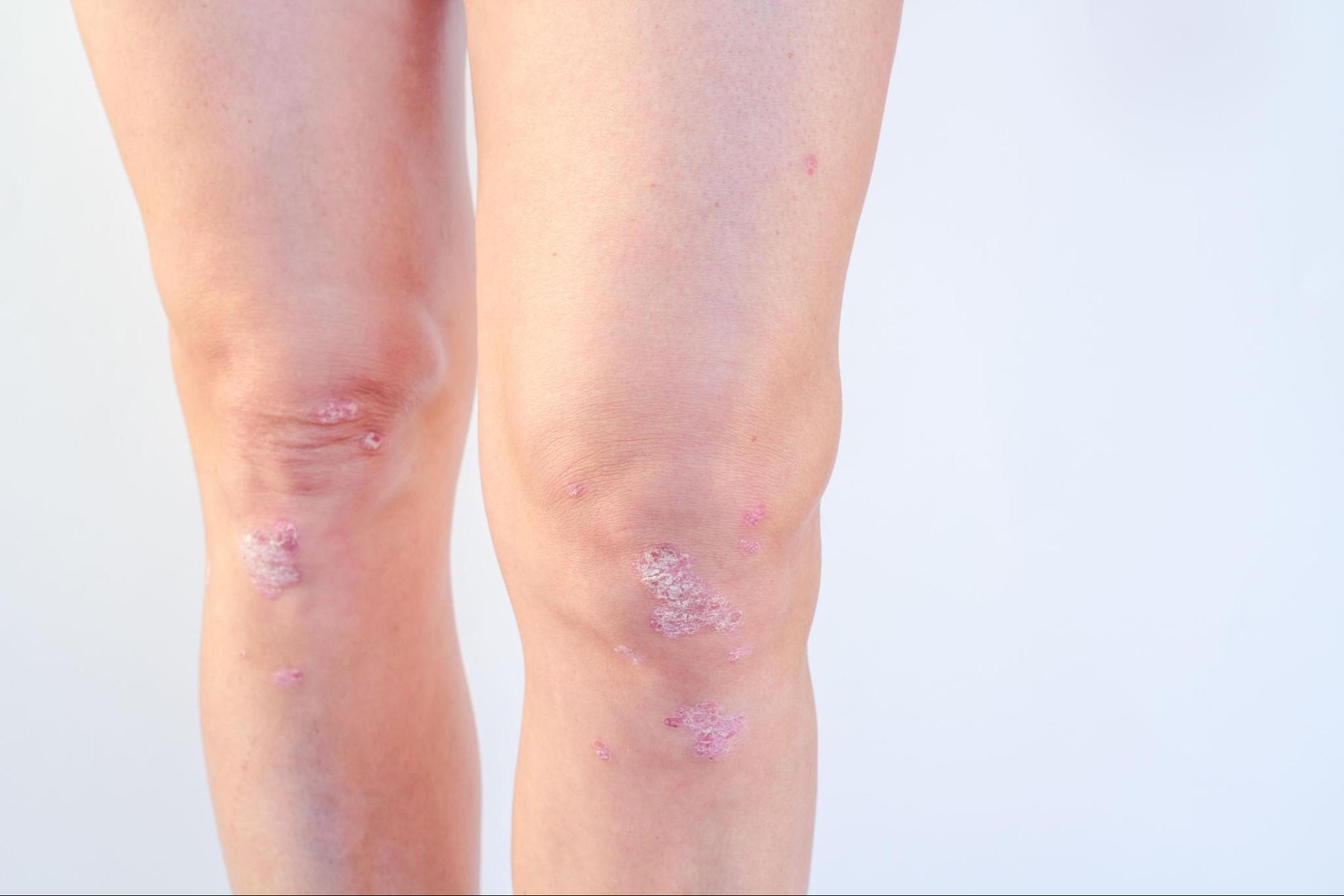
Psoriatic Arthritis (PsA) is more than a skin condition linked to psoriasis. It is a chronic autoimmune disease that can affect the joints, including the knees. When the immune system mistakenly attacks healthy joint tissue, it creates inflammation that can lead to pain, swelling, stiffness, and trouble moving.
For many adults, knee pain is often blamed on osteoarthritis. However, inflammatory conditions like PsA can also be the hidden cause. Understanding how PsA affects the knees is the first step toward finding proper treatment and lasting relief.
What Is Psoriatic Arthritis (PsA)?
Psoriatic Arthritis (PsA) is an autoimmune form of arthritis connected to psoriasis, a condition that causes patches of irritated skin. In PsA, the body’s immune system attacks the joints and surrounding tissues by mistake.
This ongoing inflammation may damage cartilage, tendons, ligaments, and bone over time. While PsA can affect many joints, the knees are a common area because they carry body weight and are essential for daily movement.
Common Features of PsA
- Joint pain and tenderness
- Swelling in one or more joints
- Morning stiffness
- Fatigue
- Nail changes
- Skin psoriasis flare-ups
How Psoriatic Arthritis Causes Knee Problems
When PsA targets the knee joint, inflammation builds inside the joint lining and nearby tissues. This causes fluid accumulation, irritation, and pain.
When the knee is in a state of chronic inflammation, the body does something counterintuitive: it grows new, fragile blood vessels (neovascularization) to bring more blood to the site. Unfortunately, these vessels bring nerve endings along with them, essentially creating a “pain highway” directly into your knee.
Key Knee Problems Caused by PsA
What’s the Difference between PsA and Osteoarthritis
Many adults assume knee pain means osteoarthritis, but the cause may be different. Because treatments differ, getting the right diagnosis matters.
|
PsA vs. Osteoarthritis Guide |
||
|---|---|---|
| Characteristics | Psoriatic Arthritis (PsA) | Osteoarthritis |
| What Causes It | Autoimmune inflammation | Wear and tear |
| Swelling | Common | Mild to Moderate |
| Morning Stiffness | Often prolonged | Usually brief |
| Warmth | Common | Less common |
| Other Signs | Psoriasis, fatigue, nail changes | Joint grinding |
Who Is at Risk for Knee Pain from PsA?
You may be at higher risk if you have:
- A history of psoriasis
- Family history of autoimmune disease
- Recurring unexplained knee swelling
- Stiffness lasting more than 30 minutes in the morning
- Pain that comes and goes in flares
- Multiple painful joints
Symptoms: When to See a Specialist
It can be difficult to tell the difference between a temporary ache and a condition that needs a doctor’s attention. However, if your knee pain includes the following “red flags,” it is time to schedule a professional evaluation:
- Persistent Swelling: If your knee is visibly swollen and the swelling doesn’t go away with rest, it could be a sign of chronic inflammation inside the joint.
- “Morning Lockdown”: If your knee feels stiff for more than 30 minutes after waking up, this is a classic sign of inflammation that needs to be addressed.
- Difficulty Moving: If you find it hard to walk, climb stairs, or even stand up, your knee’s function is being compromised.
- Pain That Won’t Quit: If rest, ice, and over-the-counter medication aren’t making a difference, the cause may be deeper than a simple strain.
- Cyclical Flare-Ups: If your pain comes and goes in intense waves—often with heat or redness—it points to an inflammatory condition that may require specialized treatment.
- The “Skin Connection”: If you have psoriasis or notice skin rashes alongside joint pain, your knee pain is likely part of a systemic issue that needs a coordinated approach.
How Diagnosis Matters in Treating Psoriatic Arthritis Knee Pain
Distinguishing between degenerative joint disease and inflammatory arthropathy requires a nuanced clinical perspective. While patients frequently present with chronic knee pain attributed to mechanical “wear and tear,” the presence of Psoriatic Arthritis (PsA) necessitates a broader assessment of systemic inflammatory markers. Clinicians look for specific phenotypic indicators that deviate from the mechanical norm:
Dermatological/Systemic Correlation: A documented clinical history of psoriasis—even if currently in clinical remission—is a primary risk factor. The presence of nail dystrophy (pitting, onycholysis) or associated systemic fatigue often serves as a clinical correlate to joint-specific pathology.
Temporal Characteristics of Stiffness: A hallmark of inflammatory arthritis is prolonged morning stiffness, typically exceeding 30 to 60 minutes. This duration distinguishes inflammatory synovitis from the briefer, movement-responsive stiffness associated with osteoarthritis.
Flare-Remission Cycles: PsA exhibits a fluctuating disease course characterized by acute inflammatory flares. These episodes present as localized edema, hyperthermia, and tenderness, distinct from the chronic, low-grade discomfort associated with mechanical degeneration.
Polyarticular Involvement: The autoimmune nature of PsA often manifests as a polyarticular presentation. When knee pain is accompanied by involvement in distal joints or a family history of autoimmune disease, the diagnostic suspicion for inflammatory arthropathy should be heightened.
Synovial Effusion: Persistent or recurrent joint effusion in the absence of acute trauma is suggestive of underlying synovitis, a condition inherently linked to the autoimmune response in PsA.
Why an Accurate Diagnosis is the Key to Relief
You might wonder why specialists insist on a comprehensive workup, including blood tests (to check for inflammation markers) and advanced imaging (like ultrasound or MRI).
The reason is simple: The right treatment depends entirely on identifying the correct cause.
If your knee pain is diagnosed as standard “wear and tear” when it is actually Psoriatic Arthritis, you might be prescribed treatments for a mechanical issue—like basic physical therapy or braces—that fail to address the underlying autoimmune attack. An accurate diagnosis ensures you are treating the root cause rather than just masking the symptoms.
Once a diagnosis is confirmed, you and your medical team can build a targeted strategy:
-
Systemic Control: Your rheumatologist can prescribe DMARDs or biologics to calm your immune system and stop the “inflammatory storm” throughout your body.
-
Targeted Joint Relief: If your systemic disease is well-managed but you still have persistent, localized knee pain, your doctor may consider interventional options like Genicular Artery Embolization (GAE). GAE targets the abnormal blood vessel growth caused by chronic inflammation, providing relief that medication alone often cannot achieve.
In short, a precise diagnosis is the prerequisite for effective care. It protects your long-term mobility by ensuring your treatment plan matches the reality of your condition.
Genicular Artery Embolization (GAE): A Minimally Invasive Approach to Knee Pain
For patients struggling with chronic, inflammatory knee pain—including cases linked to psoriatic arthritis—that has not responded to conservative treatments, Genicular Artery Embolization (GAE) offers an innovative, minimally invasive option.
What is GAE?
GAE is an outpatient procedure performed by an interventional radiologist. It is specifically designed to reduce inflammation and pain by targeting the source of the discomfort: abnormal blood vessel growth.
How It Works
- Targeting Abnormal Vascularity: Both osteoarthritis and inflammatory conditions like psoriatic arthritis can trigger neovascularization—the growth of new, abnormal blood vessels and nerve endings in the knee’s synovium. This “hypervascularity” often amplifies pain.
- The Procedure: Using a thin catheter, a specialist delivers tiny embolic particles into the genicular arteries. These particles selectively block these abnormal vessels, which helps to decrease the inflammatory signals and nerve stimulation associated with chronic knee pain.
Effectiveness and Benefits
GAE is considered an effective for many patients with moderate to severe knee pain, particularly when physical therapy, injections, or medications have failed to provide relief. Patients often report:
- Significant, measurable reductions in pain levels.
- Improved mobility and ability to perform daily activities.
- Long-lasting results, with improvements potentially sustained for over two years.
It is important to understand that while GAE is highly effective at managing pain and restoring function, it is not a cure for the underlying chronic autoimmune condition (such as psoriatic or rheumatoid arthritis). GAE treats the symptoms and the joint-specific damage caused by the inflammatory process, rather than the systemic disease itself.
Minimally Invasive Excellence: GAE at USA Pain Center
At USA Pain Center, we believe that knee pain management should be as effective as it is conservative. While traditional orthopedic approaches often point toward surgery, we prioritize minimally invasive, non-surgical alternatives that respect the structural integrity of your joint.
Why Choose a Non-Surgical Path?
For many patients, the prospect of invasive surgery—with its lengthy rehabilitation requirements, infection risks, and potential for scar tissue formation—is not the ideal first step. Our team specializes in advanced, interventional techniques that provide the same objective: significant, lasting pain relief without the need for an operating room.
These procedures offer a distinct clinical advantage:
-
Targeted Intervention: Rather than treating the entire joint, we address the specific source of pain, such as the neovascularization (abnormal blood vessel growth) that signals chronic inflammatory distress.
-
Rapid Recovery: Because these treatments are performed percutaneously (through a tiny puncture in the skin), patients often return to their normal daily activities significantly faster than with surgical alternatives.
-
Preservation of Anatomy: These procedures avoid the removal of bone or cartilage, keeping the joint’s original structure intact. This is especially important for patients who want to keep their options open for the future.
Our Commitment to Advanced Knee Health
The goal at USA Pain Center is to bridge the gap between conservative management (like physical therapy and injections) and major surgical intervention. By utilizing advanced imaging and precision-guided technology, our interventional radiologists can disrupt the pain cycle at its source.If you have been told that surgery is your only remaining option, we invite you to consult with our team. We specialize in evaluating whether your pain profile is a candidate for advanced, office-based interventions that prioritize your mobility, your time, and your long-term joint health.
Frequently Asked Questions
Can Psoriatic Arthritis affect only one knee?
PsA can affect only one knee or multiple joints, and symptoms may change over time.
Does PsA knee pain come and go?
Many people experience knee pain that “comes and goes”, called flare-ups that are followed by quieter periods.
Is knee swelling common with PsA?
Swelling is common because inflammation builds up inside the joint.
Can exercise help PsA knee pain?
Low-impact exercise often helps maintain strength and mobility, but activities should match your condition.
Is GAE surgery?
GAE is not surgery; it is a minimally invasive procedure.
Who may benefit from GAE?
Adults with chronic knee pain, often related to osteoarthritis and sometimes other conditions, may be candidates depending on medical evaluation.